The Pharmacist's Guide to Initial Resuscitation for Sepsis & Septic Shock
A note from the tl;dr team: The Surviving Sepsis Campaign updated their international guidelines for the management of sepsis and septic shock in 2026. These new guidelines update recommendations from the 2021 SSC guidelines and include 129 statements, with 46 being new statements not previously addressed.
The content in this post has been reviewed and updated in accordance with the 2026 SSC guidelines to ensure alignment with current evidence and best practices.
Steph’s Note: If you’re wondering why the title of this post doesn’t simply stop after “Sepsis,” this is the article for you. (Btw, I also would’ve thought the same thing in pharmacy school, so you’re not alone!) Here this week to explain why we all would’ve been missing a crucial bit of the sepsis story is Dr. Josef Nissan. If you don’t know Joe already from posts like this one on toxicology or from several of our handy pocket guides, you probably sense a hole in your pharmacy heart. Fill it in starting now.
I remember going through the majority of my APPE rotations using the terms sepsis and septic shock interchangeably. Then I got to my ID rotation, and my preceptor asked, “What’s the difference between sepsis and septic shock?”
We’ve hired Stanley to assist us with cheat sheet sales. We’re expecting him to be super effective, no? (Image)
You can say I struggled answering that question. But because I care so deeply about our tl;dr audience, I want you to avoid making the same mistake that I did. So strap in because we’re going for a ride on the sepsis train.
P.S. (shameless plug)! If you want a condensed cheat sheet of everything that we will go over today and more, take a look at our tl;dr sepsis cheat sheet. It has everything you need to know including pathophysiology, diagnosis, one-hour bundle, antibiotic clinical pearls, crystalloid fluid resuscitation, vasopressors, and so much more! And if you want an even more in-depth review of everything infectious diseases, take a look at our antibiotic pocket guide.
Sepsis Versus Septic Shock
Alright let’s start with the basics. So what’s the difference between sepsis and septic shock? Pretty much, one is the precursor of the other. More specifically:
Sepsis: Dysregulated systemic inflammatory and immune response to microbial infection that produces organ injury
Mortality Rate: 15-25%
Septic Shock: Sepsis with hyperlactatemia and concurrent hypotension requiring vasopressor therapy
Mortality Rate: 30-50%
Pathophysiology of Sepsis and Septic Shock
Sepsis has a very complex biochemical pathophysiology. However, this is tl;dr and let’s be real, we all want a condensed and simplified version of it. So let’s make it as basic as possible.
(Image)
For one reason or another, bacteria find their way through an organ and into the bloodstream (generally due to an untreated infection such as a UTI, pneumonia, skin & soft tissue infection, etc). And as you probably know, bacteria don’t belong in our bloodstream (duhh?).
Therefore, our body freaks out and activates numerous different pro-inflammatory and anti-inflammatory markers including cytokines, proteases, kinins, reactive oxygen species, and nitric oxide, leading to vasodilation, capillary leakage, and intravascular volume depletion. If left untreated, this can lead to severe hypotension, organ failure, and ultimately death. This cascade of events is responsible for the clinical signs and symptoms of sepsis and progression to septic shock.
Sepsis Screening Tools
Unfortunately, there is no single diagnostic test for sepsis. It is generally diagnosed using a combination of different lab tests, microbial cultures, and clinical judgment. That being said, there are two major screening tools that can be used to help identify patients with suspected infection who are at greater risk for poor outcomes. Take a look below:
2026 SSC Guideline Update: Long story short, qSOFA has fallen out of favor as a screening tool for sepsis. Here in the United States, SIRS criteria is recommended over qSOFA as a tool to screen for sepsis. And incase you want to read the guideline recommendation here you go:
“For acutely ill patients in hospital, we recommend using NEWS, NEW2, MEWS, or SIRS over qSOFA as a single tool to screen for sepsis”. Goodbye qSOFA. It’s been real.
What is the One-Hour Sepsis Bundle?
So what the heck is this one-hour sepsis bundle that I keep referring to? Well, as you have seen, sepsis is a life-threatening condition with very high mortality when not treated in a timely manner. So to make our lives easier, the Society of Critical Care Medicine (SCCM) created a one-hour bundle to help with the initial resuscitation phase for sepsis and septic shock. Here’s a brief overview of everything that we’ll talk about.
One-Hour Sepsis Bundle - Step 1 (Lactate)
So what on earth is lactate, and why is it the first step in the initial resuscitation of sepsis? Oh I am so glad you asked.
Lactate is a byproduct that is released by our organs (e.g., skeletal muscle, brain tissue, GI tract, etc) during anaerobic metabolism. So why is that helpful in diagnosing sepsis? Think about it. It helps give us an idea of organ perfusion. Still confused? Ok, let’s simplify.
Arnold does not have an issue with tissue perfusion here. (Image)
I enjoy weight lifting. So let’s use my bicep in this example. As I am sitting here typing, I am currently sepsis free. Meaning I have no bacteria in my blood and therefore no anti-inflammatory and pro-inflammatory markers are being released. So my blood pressure is currently stable, and I do not have excess vasodilation. My bicep is getting adequate oxygen from my red blood cells and is therefore undergoing aerobic metabolism.
Ok let’s flip the script.
Let’s say I now have untreated E. coli bacteremia. My body freaks out, releases a bunch of cytokines and nitric oxide, leading to severe vasodilation and capillary leakage. This severe fluid loss and vasodilation are going to cause my blood pressure to decrease. As my blood pressure continues to drop, less blood flow is going to my bicep, leading to hypoperfusion. This forces my bicep to undergo anaerobic metabolism due to the lack of oxygenation. During anaerobic metabolism, my bicep will release the byproduct lactate. Make sense now?
So as you can see, higher lactate means decreased tissue perfusion. Aka, more severe sepsis/septic shock.
One-Hour Sepsis Bundle - Step 2 (Blood Cultures)
^^How it feels when the blood cultures are drawn after antibiotics are given… :/ (Image)
Not too much to talk about here, honestly. Pretty self explanatory. With sepsis, we are concerned for bacteremia. So how can we test for it? Obtain blood cultures of course. The only important thing to remember here is ALWAYS collect blood cultures BEFORE administering antibiotics. Why? Because if you give antibiotics before, there is a chance it may eradicate the bacteria leading to false negative blood cultures. And yes, it’s officially in the updated guidelines. Take a look.
2026 SSC Guideline Update: “For adults with possible, probable, or definite sepsis or septic shock, we recommend collecting blood cultures as soon as possible and ideally before the administration of antimicrobial therapy.
One-Hour Sepsis Bundle - Step 3 (Broad-Spectrum Antibiotics)
So how do we actually treat sepsis? By getting rid of the bacteria in the blood. And how do we do that? With antibiotics of course.
Now let me start by throwing a big disclaimer at you. Each institution may differ between first-line antibiotic selection. Unfortunately there’s no standardized antibiotic selection for all patients with sepsis. There are so many different factors that come into play when selecting the best broad-spectrum antibiotic coverage. For example, everyone knows vancomycin & Zosyn (piperacillin/tazobactam), right?
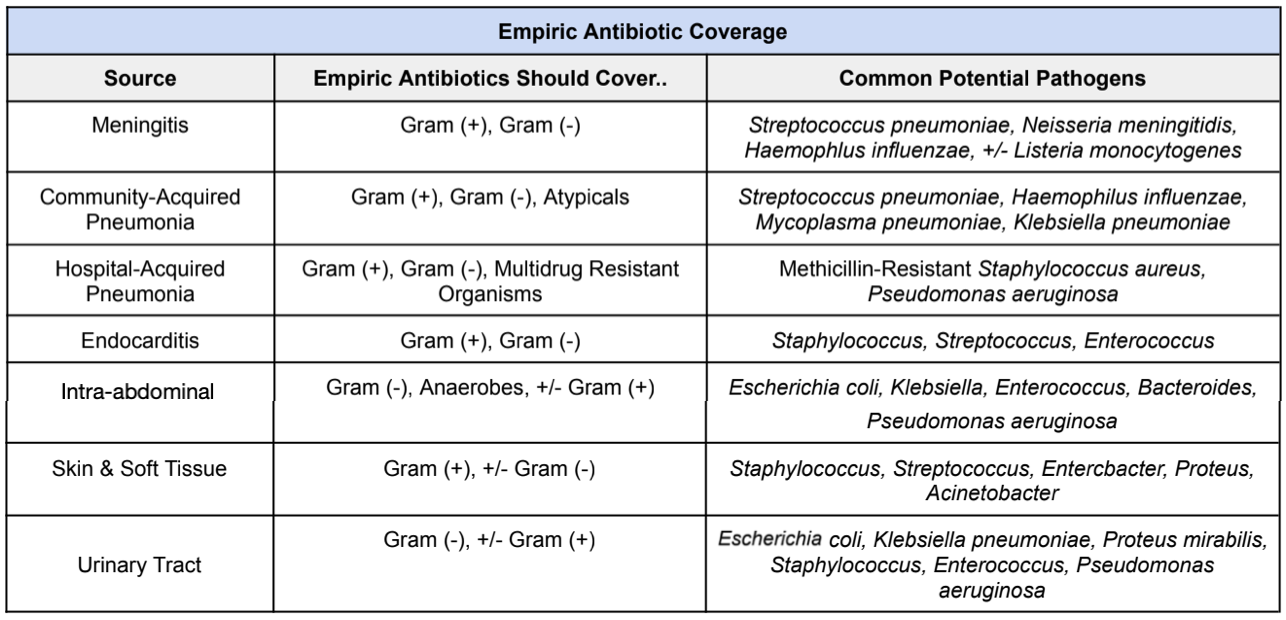
But let’s use our clinical judgment here. Does someone coming in for urosepsis without a chronic foley catheter really need to be empirically started on vancomycin? Probably not, right? So always make sure to use your clinical judgment to assess the likely source to help you figure out which empiric antibiotics should be started. A good rule of thumb to follow is:
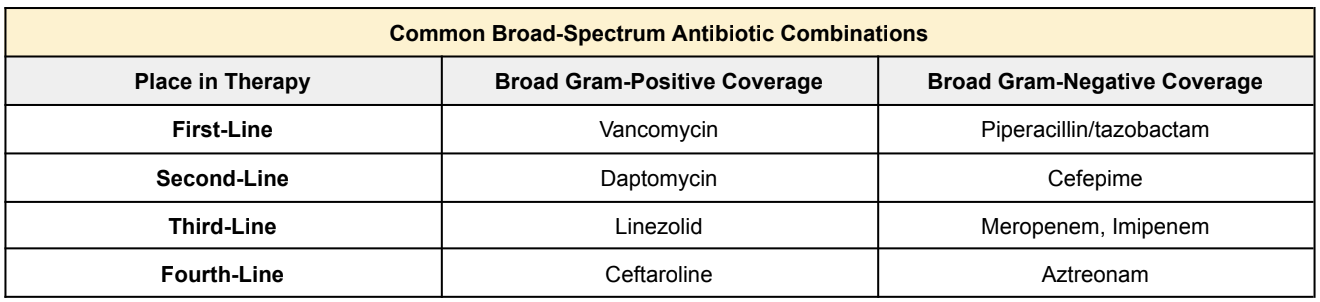
So now that we have an idea of which pathogens to empirically cover for depending on the source of infection, let’s talk about some common broad-spectrum antibiotic agents that are often used in the initial treatment of sepsis.
Again, big disclaimer here!!! Each institution may differ between first-line agent selection. It may be clinically reasonable to start antibiotics NOT listed below.
2026 SSC Guideline Updates: Okay there’s a decent amount to talk about here. Let’s go through all the super clinically relevant ones that could affect your practice.
“For adults with sepsis or septic shock at low risk of infection with a specific MDR pathogen, we suggest against using empirical antimicrobial therapy with coverage for this MDR pathogen”
“For adults with sepsis or septic shock, we suggest against using empirical antifungal therapy”
“For adults with sepsis or septic shock without risk factors for anaerobic infection, we suggest using empiric antibiotic regimen without anaerobic coverage”
“For adults with sepsis or septic shock, we recommend using prolonged infusion of beta-lactams for maintenance (after an initial loading dose) over bolus administration”
“For adults with sepsis or septic shock, we suggest de-escalation of antimicrobial therapy over no de-escalation when no pathogens are identified on final culture results”
“For adults with an initial diagnosis of sepsis or septic shock and adequate source control, we suggest shorter over longer duration of antimicrobial therapy”
Do you see the recurrent theme here? Antimicrobial stewardship at it’s finest folks. And I am HERE for it! More narrow therapy, no empiric antifungals, no need for anaerobic coverage on everybody, earlier de-escalation, and shorter duration of treatment. The one recommendation that stands out is the preference for extended infusion of beta-lactams for maintenance therapy. I have worked at a few hospitals that don’t even have extended infusion protocols. I bet you they will have to adopt them now.
One-Hour Sepsis Bundle - Step 4 (Crystalloid Fluid)
As you may remember, when we discussed the pathophysiology of sepsis, we talked about the cytokine release leading to vasodilation and capillary leakage. During capillary leakage, intravascular fluid leaks extravascularly, leading to intravascular volume depletion. Severe capillary leakage can lead to hypovolemic shock and tissue hypoperfusion. So how can we treat this intravascular volume depletion?
By giving crystalloid fluid of course!
How much fluid should we give? 30 mL/kg of IV crystalloid fluid.
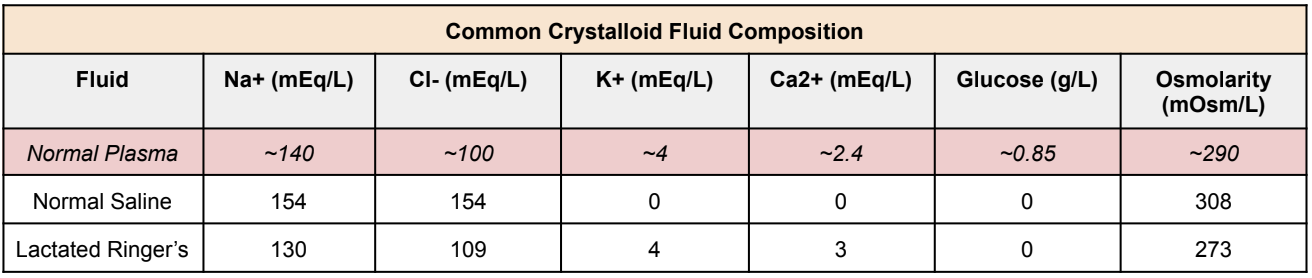
Now again, clinical judgment should be used. In septic patients with a history of CKD and heart failure, you may not need as much fluid repletion. So make sure you always assess each patient before starting fluids. That being said, the two most common IV crystalloid fluids that are used are normal saline and lactated Ringers (keep reading to find out which crystalloid is better than the other). What’s the composition difference between the two fluids? Take a look below:
P.S. If you want to learn more about fluid use in sepsis please give this article a read. It gives you a much more in-depth review of why certain fluids are recommended over others in septic patients. But if you want the quick and short version then take a look below.
2026 SSC Guideline Updates: Let’s review the new recommendations first and then we’ll summarize.
“For adults with sepsis-induced hypoperfusion or septic shock, we suggest administering at least 30 mL/kg of IV crystalloid in the first 3 hours”
“For adults with sepsis or septic shock, we recommend using crystalloids as first-line fluid for resuscitation”
“For adults with sepsis or septic shock undergoing initial resuscitation, we suggest using balanced crystalloids over 0.9% saline”
“For adults with sepsis or septic shock, we suggest using crystalloids alone over crystalloids with supplemental albumin for fluid resuscitation”
“For adults with sepsis and septic shock, we recommend against using starches for resuscitation”
For adults with sepsis and septic shock, we suggest against using gelatin for resuscitation”
Moral of the story is crystalloids > colloids, balanced crystalloids (e.g. LR, plasma-lyte) > normal saline. So folks, please resuscitate septic patients with 30 mL/kg of either LR or plasma-lyte.
One-Hour Sepsis Bundle - Step 5 (Vasopressors)
Ah, my favorite part :). Again, this all comes back to the pathophysiology of sepsis. Bacteria in the blood → cytokine & nitric oxide release → vasodilation & capillary leakage → hypotension → tissue hypoperfusion → death. You got it? Ok, good.
So, when do we start vasopressors? ONLY if the patient remains hypotensive during or after fluid resuscitation to maintain a MAP ≥ 65 mmHg (take a look below regarding MAP nuance updates). Why do we aim for a MAP greater than 65 mmHg?
It’s not random. The most important organ in the body is the brain (you can argue with me though). So a MAP of 65 mmHg is the minimum vascular pressure that is needed to continue to perfuse the brain. Anything less than that leads to brain hypoxia and death. So now you know why we aim for this seemingly arbitrary number.
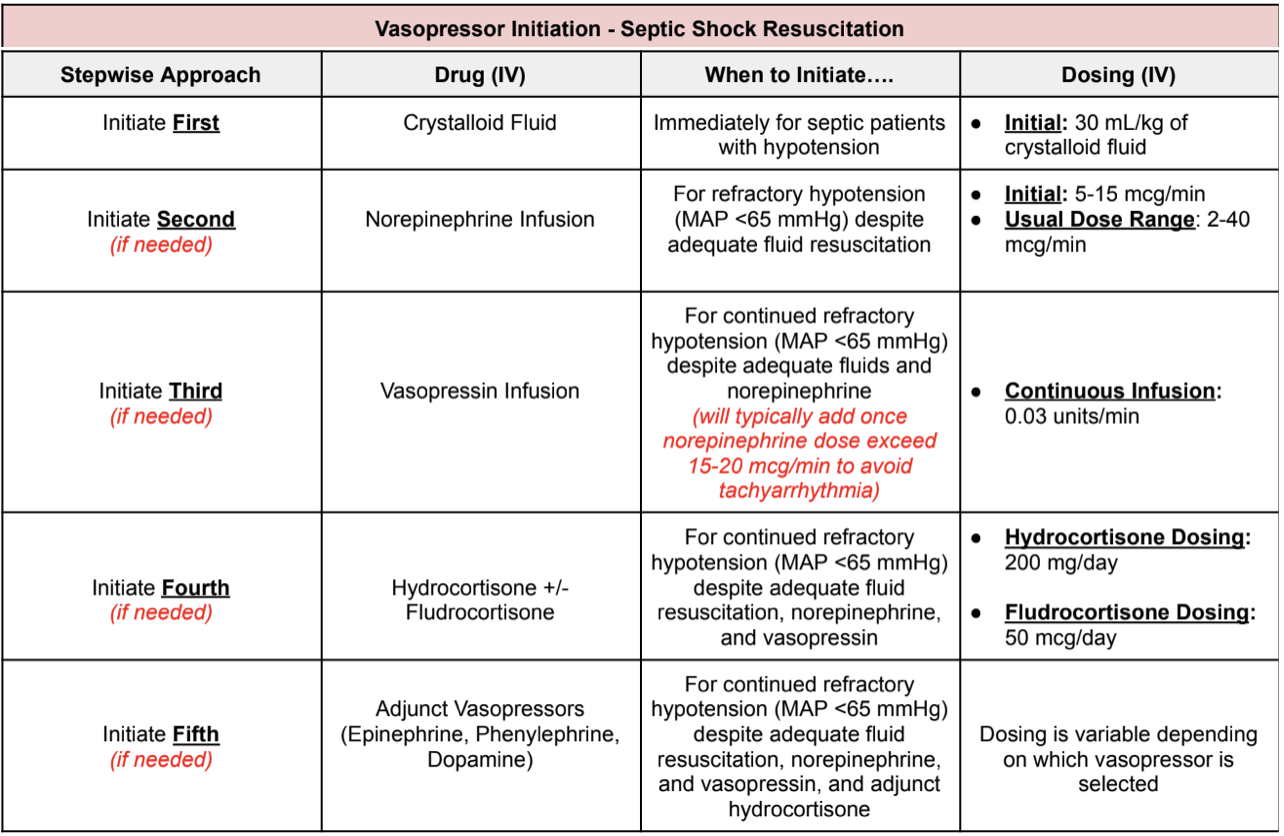
Ok, so which pressors do we start? Well, I made a table for you that makes it pretty easy to follow. Take a look:
Now we know when and which vasopressors to start for patients with refractory septic shock. Let’s say you did a miraculous job and the patient’s blood pressure has improved immensely. So how do we peel back on vasopressors? Go backwards of course.
For example let’s say you have patient JJ who came in for septic shock secondary to CAP. JJ was given IV fluids and was started on norepinephrine, vasopressin, hydrocortisone, and phenylephrine. If MAP has continued to improve, start by taking off phenylephrine → then hydrocortisone → then vasopressin → then norepinephrine. Pretty simple, right?
2026 SSC Guideline Updates: There’s a a few things to talk about here. Let’s go through them.
“For adults with septic shock, we recommend an initial MAP target of 65 mmHg over higher MAP targets”
“For adults with septic shock 65 years old or older, we suggest an initial MAP range of 60-65 mmHg over higher ranges”
“For adults with septic shock and inadequate MAP levels despite norepinephrine and vasopressin, we suggest adding epinephrine”
“For adults with septic shock and ongoing requirement for vasopressors, there is insufficient evidence to make a recommendation on use of oral midodrine”
Long story short, lower MAP goals may be appropriate in critically ill elderly patients, epinephrine is the recommended third pressor to add, and they plead the fifth regarding use of oral midodrine in septic patients.
Questionable Adjunct Therapy - Vitamin C, Vitamin D, and Probiotics
This obviously isn’t part of the one-hour bundle but I wanted to add it given the recent guideline updates. After years of arguing, the SSC guidelines finally made a stance against some of the voodoo therapy for sepsis and septic shock. I will keep this section concise as we’ve already gone through a lot of information.
2026 SSC Guideline Updates:
“For adults with sepsis or septic shock, we suggest against using IV vitamin C in patients with sepsis or septic shock”
“For adults with sepsis and septic shock, we suggest against using vitamin D therapy for sepsis treatment”
“For adults with sepsis or septic shock, we suggest against using probiotics”
Nicely put, please don’t use vitamin C, vitamin D, or probiotics to treat sepsis and septic shock. Thanks :)
The tl;dr of Sepsis & Septic Shock
Sepsis and septic shock are not the same thing. Untreated sepsis can lead to septic shock.
Sepsis: Dysregulated systemic inflammatory and immune response to microbial infection that produces organ injury
Septic Shock: Sepsis with hyperlactatemia and concurrent hypotension requiring vasopressor therapy
Bacteremia leads to the activation of numerous different pro-inflammatory and anti-inflammatory markers including cytokines, proteases, kinins, reactive oxygen species, and nitric oxide leading to vasodilation, capillary leakage, and intravascular fluid depletion. If untreated, this can lead to severe hypotension, organ failure, and ultimately death. This cascade of events is responsible for the clinical signs and symptoms of sepsis and progression to septic shock.
There is no single diagnostic test for sepsis. It is generally diagnosed using a combination of different lab tests, microbial cultures, and clinical judgment. Common diagnostic screenings to help diagnose sepsis include the qSOFA & SIRS screening.
The Society of Critical Care Medicine recommends the following one-hour bundle for the initial resuscitation of sepsis/septic shock:
Step 1: Measure lactate level
Lactate is a byproduct released during anaerobic metabolism. Increase in lactate means increase in tissue hypoperfusion
Step 2: Obtain blood cultures BEFORE administering antibiotics
Step 3: Administer broad-spectrum antibiotics
Always use clinical judgment when starting broad-spectrum antibiotics
Step 4: Begin rapid administration of 30 mL/kg of crystalloid fluid for hypotension or lactate ≥ 4 mmol/L
A goal MAP of 65 mmHg is recommended to ensure appropriate brain perfusion. In septic patients 65 years old or older, an initial MAP target of 60-65 mmHg is recommended
Patients with obvious hypovolemia should be resuscitated with 30 mL/kg of IV crystalloid therapy
Step 5: Initiate IV vasopressors if hypotensive during or after fluid resuscitation to maintain a MAP ≥65 mmHg
Always use the following algorithm when starting vasopressors for the treatment of septic shock:
Initiate first: crystalloid fluids (balanced crystalloids recommended over normal saline)
Initiate second: norepinephrine
Initiate third: vasopressin
Initiate fourth: hydrocortisone +/- fludrocortisone
Initiate fifth: epinephrine
Initiate sixth: other adjunctive pressers, including phenylephrine, dopamine, and angiotensin II