The Official Warfarin "Oh Shit" Drug Interaction List
A note from the tl;dr team: this article was reviewed and updated in October 2025 to ensure accuracy and relevance
If you are a future (or current) pharmacist, you need to know warfarin. You don't need me to tell you that. Every teacher and preceptor you've had since you started school has been drilling that into your head.
However, you've probably also noticed that few will actually tell you how to dose warfarin. Sure, you learn about purple toes and birth defects, but that doesn't tell you what to do when your patient's INR is 5.6.
The reason everyone dodges warfarin dosing like Floyd Mayweather is because it's tricky and complicated. Patients respond differently to warfarin due to genetic factors. Everything from green tea to Lipitor can affect the INR.
All of the things interact with warfarin. Your job as a pharmacist is to determine how to manage it.
After the NAPLEX, you have to do more than just recognize a drug interaction exists with Cipro--you have to fix it for your patient. That's going to be our subject today. But because there are so many drug interactions with warfarin, we are only going to talk about the worst of the worst.
This "Oh Shit" list is a collection of situations where you practically guarantee that you'll have to adjust the warfarin dose. You may even adjust the warfarin dose empirically.
How does this apply to school? Let's say you're taking a test (or on rotation), and your patient starts (or stops) one of the drugs below. The correct answer is NOT going to be "continue current dose and check the INR in 7 days." You'll need to make an immediate adjustment to the warfarin dose (and then still check the INR in a couple of days).
This is different from most of the other warfarin drug interactions you know. It's a somewhat rare case to make such immediate and drastic changes to therapy. More often than not, you'll just monitor the INR more closely and make adjustments as necessary.
To be clear, when we talk about warfarin dose adjustments below, we are talking about the total weekly dose of warfarin.
Also, please remember that this article is for informational purposes only. These recommendations are author opinion and do not reflect any specific source of guidelines. Please continue to use sound clinical judgment when managing your patients. Please see our website disclaimer for more information.
Also, if you want to get REAL comfy and cozy with warfarin…check out our magnum opus - Warfarin: The Definitive Guide. Or, if you want something that’s a little less in depth, check our this article that covers the bare essentials of dosing warfarin.
The Basics of Warfarin Drug Interactions
Before we go over the “Fab Five” that make up the “Oh Shit” list, let’s review the kinetics of warfarin to help us understand why these drug interactions occur in the first place.
For starters, warfarin is a substrate of CYP2C9 (major), 1A2 (minor), and 3A4 (minor). Now that’s a lot of CYPs. So, long story short, any drug that inhibits or induces any of those CYP enzymes can theoretically interact with warfarin and cause all kinds of INR fluctuations.
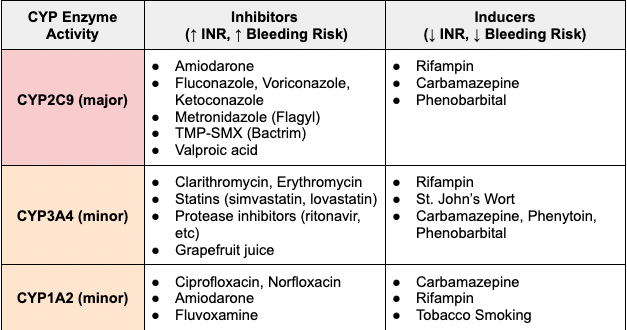
Now we can’t go over every single drug, herbal product, or food that interacts with warfarin. If we did, you’d be reading this article for the next 7 days. Instead, here is a table I made that highlights all the common drugs you want to avoid and why.
Oh, and one more nerdy fun fact about warfarin drug interactions. As we can see above, certain antibiotics have CYP enzyme inhibition which can lead to drug-drug interactions with warfarin. But that’s not the only mechanism in how antibiotics can lead to increased INR.
Believe it or not not, our normal healthy gut bacteria produce vitamin K which reduces the effects of warfarin. When we take antibiotics, our normal gut flora may be disrupted (hence why we normally educate about nausea, diarrhea, vomiting with oral antibiotic use). Anyway, this disruption may lead to reduced vitamin k production causing an increase in INR. Pretty gnarly right?
Okay, now back to our “Fab Five”.
Bactrim (TMP-SMX)
There is really no more "classic" drug-drug interaction than Bactrim and Warfarin. It just hits on so many levels. They go together like Chinese food and chocolate pudding. Like skateboarding and freeway ramps.
Bactrim inhibits CYP 2C9; which you remember is responsible for breaking down the more potent S-isomer of warfarin. Bactrim also inhibits CYP 3A4; which you remember is responsible for breaking down the less potent R-isomer of warfarin. Bactrim can also (somewhat) disrupt the normal flora in the gut; which you remember is responsible for breaking down and getting vitamin K into your body. Finally, Bactrim is very highly protein-bound and can displace warfarin from the albumin it's bound to in your patient's blood (more on that below).
Indeed, Bactrim is the Sabretooth to warfarin's Wolverine.
You will probably reduce the warfarin dose by about 50% for patients starting Bactrim. In higher-risk, more sensitive patients, you may even hold a dose of warfarin and then reduce it.
Amiodarone
Let's just make a nice and tidy list to cover amiodarone.
Strong CYP 2C9 inhibition
Moderate CYP 3A4 inhibition
Frequently used to manage a-fib---and a-fib patients need anticoagulation to prevent strokes (so amiodarone and warfarin are commonly used together)
Stupidly long half-life (~56 days)
That half-life is a real doozie, too. That means that a drug interaction between amiodarone and warfarin can happen several months after a patient has stopped taking amiodarone. Pro tip: That's a favorite test question in pharmacy school. Also, for honorable mention, don't forget that amiodarone can cause blue discoloration of the skin and fingernails--so don't confuse it with the purple toe that warfarin can cause.
Because of the kinetics of amiodarone, this is a complex mechanism. It can take a while for amiodarone to be at steady state. If you already have a patient stable on warfarin and you are starting amiodarone, you may actually wait a few days before decreasing the warfarin dose. But in the end, you will usually reduce the warfarin dose by about 50% for patients starting amiodarone. If a patient is already stable on amiodarone and you are starting warfarin, use half of the dose you ordinarily would.
Flagyl (Metronidazole)
The mechanism with Flagyl is not that well defined, but it appears to be mostly due to CYP 2C9 inhibition. There is also the potential for disruption of gut flora. It's not like a cephalosporin, which is basically like a smart bomb against the poor bacteria that help you absorb vitamin K.
But there's a slight chance that metronidazole could disrupt gut flora. Remember that warfarin specifically inhibits vitamin K-dependent clotting factors (II, VII, IX, X, Protein C, Protein S). If there is less vitamin K, there are less of those clotting factors. All of this means that Flagyl can shoot up your patient's INR.
Expect about a 25 - 30% reduction in the weekly warfarin dose for the duration of Flagyl therapy.
Fluconazole, Voriconazole, Ketoconazole
There isn't a whole lot to explain with this one--just some strong CYP 2C9 inhibition along with a dose of moderate CYP 3A4 inhibition. You're probably starting to notice a trend with 2C9 and 3A4 inhibition by now. Congratulations! You can now apply this knowledge to any other inhibitors you come across.
In most cases, you'll reduce the weekly warfarin dose by about 40% with fluconazole, voriconazole, and ketoconazole. If the patient's INR is on the higher side of their target range to begin with, you may even consider holding a dose of warfarin before starting the dose reduction.
Rifampin
If you get nothing else out of this article, I want it to be that rifampin is the most powerful CYP inducer known to man. Like seriously. You have to look out for rifampin on every test. It is a red flag with a roman candle and a bullhorn screaming at you to be on the lookout for drug interactions.
When you start practicing, if you are ever managing a TB patient, you will see the havoc that this little gem can cause on concurrent drug therapy. Especially because patients who get TB are usually immunosuppressed and on a cocktail of drugs as it is.
You'll come across someone who is 4 months post-op from a liver transplant and taking tacrolimus. They'll develop TB and need to start RIPE. Have fun!
In terms of warfarin, you may literally have to do anything from 2x to 5x the dose if your patient starts rifampin. It's that profound. Also, remember the fun little NAPLEX fact that rifampin can give your patients red-orange secretions (urine, tears, sweat).
Keep that in mind because if your patient is peeing red you need to determine if it's the rifampin or if they are bleeding from the warfarin.
Honorable Mention: Phenytoin
Phenytoin deserves a place on this list because it just does wacky shit with warfarin. It's possible you will not need to empirically change the warfarin dose based on phenytoin initiation, but you will definitely need to harass your patient by monitoring the ever-loving crap out of them for the first couple of weeks.
So first, you may remember from pharmacology that warfarin is highly protein-bound. This means that a lot of it is "inactive" as it's floating around your bloodstream because it is tied up and bound to your serum albumin. Quick side note: This is also why your warfarin patients with low albumin require smaller doses to achieve therapeutic INRs.
However, phenytoin is more protein-bound than warfarin. When you start phenytoin, the first thing it does is kick a bunch of warfarin off of your serum albumin--essentially "activating" it. This will raise your patient's INR. It will usually normalize in a few days.
But we're not done yet. Remember that phenytoin is a pretty strong CYP inducer across the board. So even while it's kicking warfarin off of albumin, it's ramping up production of 2C9 and 3A4--increasing the metabolism of warfarin. This will lower your patient's INR.
You just have to monitor phenytoin carefully, as it's likely every patient will respond differently. In general, expect an initial increase in INR, followed by a decrease about a week or so later. Once you get the patient therapeutic and stable on phenytoin, the drug interaction should normalize.
Foods that Interact with Warfarin
Lastly, let’s not forget diet when looking at warfarin interactions. Foods high in vitamin K can greatly affect warfarin dosing as they make it less effective. Because of this, it is important to tell patients to keep their diet consistent and to be aware if they make any changes, with the following foods being common suspects:
Foods high in Vitamin-K
The End
Although warfarin interacts with everything on this lush green earth of ours, these are the interactions that really need to give you pause. While every patient and scenario is different, most of the time, a healthy dose of additional monitoring will guide your warfarin dosing decisions when new drugs are added or taken away.